There are three types of cancer only men can suffer from – testicular cancer, prostate cancer and penile cancer. We have supplied information on all three of these disorders, which may help you to detect early signs of the disease.
What are the testicles?
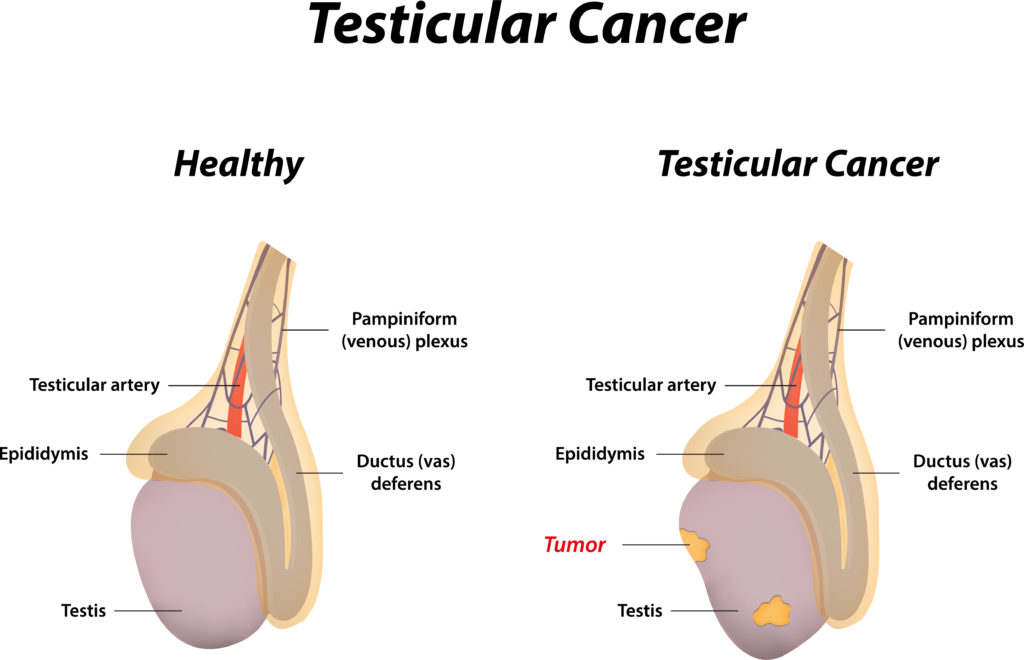 The testicles are the male sex gland, they are two small oval shaped organs located inside the scrotum, the loose bag of skin that hangs below the penis. From the age of puberty the testicles produce sperm, which can fertilize the female egg after intercourse.
The testicles are the male sex gland, they are two small oval shaped organs located inside the scrotum, the loose bag of skin that hangs below the penis. From the age of puberty the testicles produce sperm, which can fertilize the female egg after intercourse.
The testicles also produce the male hormone testosterone. This hormone is responsible for male characteristics, such as a deep voice, beard growth, muscle development and the ability to have an erection.
What is testicular cancer?
Testicular (or testes) cancer is now the most common form of cancer in younger men occurring mostly in those aged between 15 and 40. However, it is still quite rare with just over 1,500 new cases a year (around 1 in 400). Testicular cancer is also one of the most curable cancers. Over 90% of patients make a full recovery when the disease is caught at an early stage.
What causes testicular cancer?
Testicular cancer occurs when cells in the testicle grow in an abnormal way and form a tumour. The exact cause of testicular cancer is still unknown. In unborn male children, the testicles develop inside the abdomen between the kidneys and descend into the scrotum before or shortly after birth. Testicular cancer is known to be common in men who have a testicle which has failed to descend.
Am I at risk of getting testicular cancer?
Potentially all men are at risk. However, the following factors may increase the risk of you developing testicular cancer:
There is not known to be any link between injury or sporting strains and testicular cancer.
What are the symptoms of testicular cancer?
The most common symptom of testicular cancer is swelling with or without pain in part of a testicle. Some people may notice an ache in their lower abdomen. There may be a feeling of ‘heaviness’ in the scrotum. In a few people the testicle suddenly becomes swollen and very tender. You may also notice blood passing from the penis or blood in urine. Testicular cancer usually affects only one of the testicles.
The symptoms of testicular cancer should not be ignored, but unfortunately, ignorance, fear and embarrassment may all cause men to delay in seeking medical advice. However, all of these symptoms occur far more often for reasons other than cancer. If you have any symptoms you are unsure about you should always contact your doctor for advice.
Self examination
A good way of detecting the disease when it’s still in it’s early stages is for men to examine their own testicles. You should regularly carry out a self-examination (once a month) from the time of puberty onwards. This will help you to know what is normal for you (everyone is different) and you will be able to detect any changes early on. You could always ask your partner for help.
The best time to examine your testicles is after a warm shower or bath, when the skin of the scrotum is relaxed. It is very rare for cancer to develop in both testicles, so if you are unsure about a lump, you can usually check for a possible change in one testicle by comparing it with the other testicle, to see if they feel or appear the same.
Whilst standing, support your testicles in the palm of your hand, this allows you to use the thumb and fingers of both hands to examine the testicles. Become familiar with the size and weight of each testicle. It is not unusual to have one testicle slightly larger or hang lower than the other. However, any recent changes in size or weight may mean that something is wrong.
Next, examine each testicle individually. Using both hands, gently roll the testicle between the thumb and fingers. Press gently to check for any lumps, swelling or tenderness. If you press too hard it will be painful. Normally testicles will feel smooth without any lumps. Also, check the testicles for any change in firmness. If you feel a soft tube at the top and back of the testicle, don’t worry this is the epididymis, which stores and carries sperm and should not be confused with an abnormal lump.
REMEMBER: If any of the warning signs are present when you perform your examination you should seek medical advice as soon as possible. Try not to panic, these symptoms are usually caused by other less serious conditions. Most lumps found in self examination are benign.
How is testicular cancer diagnosed?
The doctor will usually begin by giving you a full physical examination, if the doctor suspects you might have testicular cancer, he/she will refer you to a hospital for further tests. Tests you might have include a ultrasound, CT scan, urine and blood tests. A biopsy is not recommended for diagnosing testicular cancer as it can encourage the disease to spread. Therefore, the only way to confirm that cancer is present is to remove the affected testicle. The testicle will then be analysed under a microscope.
What treatment is available for testicular cancer?
If testicular cancer is diagnosed and it has not spread beyond the testicle, surgery to remove the testicle may be the only treatment required. The type of treatment you receive will depend on how far the cancer has spread, your age and general health. You may need to have radiotherapy with surgery to ensure the cancer cells have been killed and to prevent it from spreading. Chemotherapy may also be used to treat testicular cancer.
What are the after effects of treatment?
As previously mentioned, it is rare to have the disease in both testicles, and if one testicle has to be removed, the remaining testicle tends to make enough sperm to compensate for the loss. The removal of a testicle will not affect your sex life and ability to father children. However, some men may experience a period of 12-24 months with reduced fertility.